Important! We have changed our site host. Please update your bookmarks. Old ones no longer work. The Search currently doesn't work but will when Google reindexes pages.
Our most recent book has answers to the 200 most common questions that readers have asked us over the 19 years since this site began. Get it here: Your Diabetes Questions Answered
Blood Sugar Throughout the Day for Normal People and People with Diabetes
Most of us have heard the term blood sugar bandied around enough that we think we know what it means, but few of us really understand the complexity of the system that makes a steady supply of fuel available to our cells around the clock.
The basic facts are these: All animals have a small amount of a simple sugar called glucose floating around in their bloodstream all the time. This simple sugar is one of two fuels that the cells of the body can burn for fuel. The other is fat. Though you may occasionally eat pure glucose--it's called "dextrose" when it is found in the list of ingredients on a U.S. food label--most of the glucose in your blood doesn't come from eating glucose. It is produced when your digestive system breaks down the larger molecules of complex sugars and starch. Sugars like those found in table sugar, corn syrup, milk and fruit and the starches found in flour, potatoes, rice, and beans all contain chains of glucose that are bonded together with other substances. During digestion, enzymes break these bonds and liberate the glucose molecules which are then absorbed into your bloodstream.
How Blood Sugar is Measured
Blood sugar concentrations are described using a number that describes the weight of glucose that is found in a specific volume of blood. In the U.S. that measurement is milligrams per deciliter, which is abbreviated as "mg/dl." Europeans and almost all researchers publishing in medical journals use a different measurement, micromoles per liter, abbreviated "mmol/L."
You can convert any European measurements you encounter to the American standard by multiplying the mmol/L number by 18. There's a handy converter online that will do this for you automatically. You'll find it at http://www.childrenwithdiabetes.com/converter.htm
If a blood test says that your blood sugar is 85 mg/dl this means that there are 85 milligrams of glucose in every deciliter of your blood. This would mean that each liter of your blood would contain 850 milligrams or .85 of a gram of glucose. The body of typical person weighing 150 pounds contains about 4.7 liters of blood. So if their blood sugar has been measured at 85 mg/dl, at the moment they were measured, they had a total of 4 grams of glucose circulating in their bloodstream. This would be 16 calories worth of glucose or as much glucose as there is in two "Sweetart" brand candy discs.
How Your Blood Sugar Levels are Regulated
However, the concentration of glucose in your blood is never static. Your cells are constantly slurping up that blood glucose and burning it for fuel, forcing your liver and pancreas work full time to replace it. Replacing the glucose removed from your bloodstream is essential. It almost as important as keeping the level of oxygen in your blood just right. This is because your brain requires a small but steady supply of glucose at all times and will stop functioning if it doesn't get it. So sensitive is your brain its need for glucose that if the concentration of glucose in your blood stream goes below 30 mg/dl (1.7 mmol/L) you may become unconscious or even die.
Fortunately, there are a number of robust processes built into your metabolism that prevent this from ever happening. Unless you have one of a few extremely rare tumors that affect your glands or are taking one of the few drugs that cause your body to secrete insulin whether or not it is needed, you need never worry that your blood sugar will ever drop anywhere near low enough to cause unconsciousness. A complex set of metabolic processes orchestrated by your pancreas, liver and brain release a constant stream of glucose into your bloodstream at all times. If the systems that regulate your blood sugar are completely normal, the amount of glucose they release is just enough to replace the glucose your cells have removed and burnt for fuel. If they are not, the amount of glucose released might be more than enough, but it will never be life-threateningly less.
Your body gets this replacement glucose from several different sources. Most of the starch and sugar you eat turns into glucose when it is digested. This glucose goes right from your digestive system your bloodstream. Some of the glucose you can't burn off immediately is converted into a storage form called "glycogen" and stored in your liver and muscles. Average bodies can store about 190 grams of glycogen, though some interesting but long-neglected research has found that some people store a great deal more. That typical 190 grams of glucose is worth 360 calories. The body can draw on it anytime it needs some extra glucose fast.
If you were to burn off all this stored glycogen, your body would still be able to ensure that there was enough glucose circulating in your bloodstream at all times by switching into a mode where most of your cells start burning fat instead of glucose. Then to provide the small amount of glucose that your neurons need, since those brain cells are the only ones in your body that can't burn fat, your liver would transform protein into glucose. This protein might come from protein foods you ate--meat or cheese, for example. But if you were unable to eat, or did not eat enough protein, the protein needed to provide the brain its glucose would be taken from your own muscle tissue. It is because your body can "eat" your muscle tissues in this way that starvation diets and diets that are too low in protein result in a dangerous loss of muscle tissue.
The Fasting and Post-Meal Blood Sugar State
Though blood sugar concentrations fluctuate throughout the day, they can be divided into two basic states. One is the fasting state and the other is the post-meal state. The term "post-meal" is latinized English for "after dining" and refers to the period that follows after you have eaten food.
The Fasting State
You are in the fasting state any time when digestion has been completed. It occurs at night while you sleep. You may also enter the fasting state three hours after you have last eaten. However, if you snack between meals and after dinner you may not re-enter the fasting state while you are awake.
In the fasting state your liver keeps your blood sugar concentration at a normal level by continually releasing small amounts of glucose from the glycogen it has stored after meals or by producing new glucose from protein.
The concentration of the hormone insulin in your blood is the signal which tells the liver whether it needs to dump glucose into the blood. Insulin is released by special cells in the pancreas, the beta-cells, when they sense a rising level of glucose in the blood. When there is no new glucose coming into the blood stream from digestion, little insulin is released.
A normal, healthy liver is also sensitive to insulin levels. The less circulating insulin it senses in the blood stream, the harder the liver will work to put more glucose into the blood. In a healthy person, the liver keeps the fasting blood sugar concentration near 85 mg/dl (4.7 mmol/L) at all times.
The Post-Meal State
You remain in the fasting state until you eat some food containing carbohydrates. After eating, any pure glucose that was present in your food will be absorbed into your bloodstream within fifteen minutes. Other carbohydrates will require digestion. Those that digest quickly--the so-called "high glycemic carbs" like white flour or sugar--typically take between a half hour and an hour enter your bloodstream. Slower acting carbohydrates like whole grains or pasta may take an hour to two or even, in the case of some hard-wheat pastas, three hours to release their glucose into your blood.
During this post-meal state, the concentration of glucose in your blood will begin to rise as the glucose liberated from your food comes pouring in. But in a healthy body, this rise is brief and not very high.
That is because as soon as the concentration of glucose in your body starts to rise, it stimulates the insulin secreting cells in your pancreas, called beta-cells, to produce a large burst of a hormone called insulin. Insulin's function is to activate receptors on your body's cells. This enables these cells to remove the circulating glucose molecules from your bloodstream and either burn them for fuel or store them for future use.
Insulin
Insulin is powerful stuff. To get an idea of how powerful, consider this. If a person who weighed 140 lbs made no insulin at all, every gram of carbohydrate they ate would raise their blood sugar by 5 mg/dl (.3 mmol/). That means if they were to eat a typical coffee shop bagel which contains about 60 grams of carbohydrate, the glucose in that bagel would raise their blood sugar some 300 mg/dl (16.7 mmol/L). If their fasting blood sugar was a normal 85 mg/dl before they ate that bagel, by the time they had finished digesting it their blood sugar would rise to a whopping 385 mg/dl (21.4 mmol/L).
But in a normal person that doesn't happen. If a person with normal blood sugar control were to check their blood with a portable blood sugar meter every ten minutes throughout the three hours that followed their first bite of that bagel, the highest blood sugar concentration they'd be likely to see would almost certainly be under 140 mg/dl (7.8 mmol/L)--and perhaps a lot lower. This blood sugar peak would probably occur about half an hour after they ate the bagel. By an hour after they'd eaten their bagel their blood sugar would probably have dropped to a value near 100 mg/dl (5.6 mmol/L), though it might even have sunk back even lower, to their fasting value of 85 mg/dl. In any case, two hours after they'd eaten, the whole 60 grams of carbohydrate present in the bagel--an amount that could have raised their blood sugar some 300 mg/dl if they did not produce insulin--would have been hustled off into their cells without making a significant change in their blood sugar concentration. That's what insulin can do.
Diabetic Post-Meal Blood Sugar Response
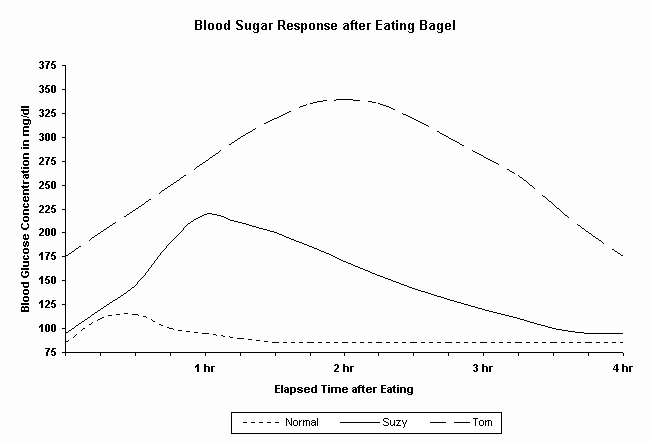
Now let's look at an example of what happens when a person's blood sugar is not normal. Suzy and Tom both have abnormally high post-meal blood sugars. Both meet the diagnostic criteria for type 2 diabetes, though because Suzy's fasting blood sugar is normal, her doctor would probably tell her that she is normal or perhaps that she is prediabetic. Tom's blood sugar has deteriorated so badly his doctor would diagnose him as diabetic based solely on a fasting test.
If Suzy and Tom were to each eat a bagel containing 60 grams of carbohydrate, about half an hour after they ate that bagel, the concentration of glucose in their bloodstreams would also start to climb. But unlike what happened to our normal person, it would not start coming down half an hour after they ate. Instead, their blood sugar concentrations would go higher and higher until it would eventually reach a peak.
Suzy and Tom would experience differing peak concentrations and they may occur at different times after they eat even though could be diagnosed with the same disorder--Type 2 diabetes. That is because their bodies produce different amounts of insulin and their cells also differ in how well they can respond to that insulin. An hour after eating the bagel, the concentration of glucose in Suzy's blood might rise to 220 mg/dl, while Tom's blood sugar might rise to 275 mg/dl. During the second hour after eating, Suzy's blood sugar might drift down to 180 mg/dl, while Tom's might keep climbing to 340 mg/dl --a value very close to that which a person would reach if their body produced no insulin at all.
During the third hour, Tom's blood sugar might finally start coming down while Suzy's would be close to a normal value. Finally, four long hours after eating the bagel, assuming they'd had nothing else to eat, Suzy might have a blood sugar concentration of 98 mg/dl, which is also the fasting level she noted when she measured her blood sugar the first thing in the morning. Tom's blood sugar might be much higher at 165 mg/dl. This is much higher level than Suzy's fasting level, but it is lower than Tom's fasting level which is a relatively high 175 mg/dl.
Even though Suzy and Tom's post-meal blood sugar values reach levels high enough to be diagnosed as diabetic, they do eventually come back down. Because they end up a lot lower than the 385 mg/dl level their blood sugars would have reached if their bodies did not produce any insulin at all, it's clear that that their bodies are still producing some insulin, though it is just as clear, especially in Tom's case, that insulin is not working very well.
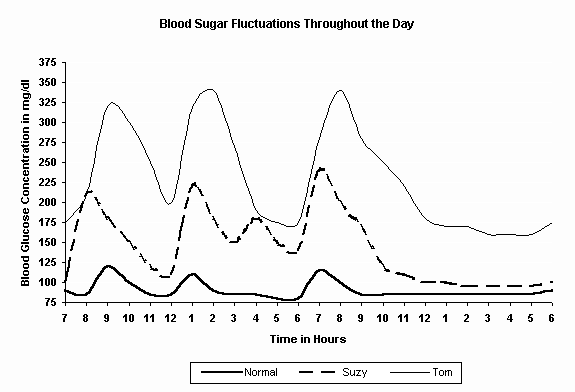
The graph below shows how blood sugar in people like this might behave through and entire day.